MEN’S HEALTH MONTH: A New Era in Oral Testosterone
We are excited to kick off this month by introducing a groundbreaking advancement in testosterone treatment: Kyzatrex, a revolutionary new oral testosterone therapy

By Dr. Emeka Ofobike, Jr. MD, FAAOS
When I started writing this post, it was Monday 7/26 and I was lying in an ICU bed on the 10th floor of the University of Colorado hospital in Denver breathing 80% oxygen through a positive airway pressure mask. I had been diagnosed with a presumed case of acute altitude sickness known as High Altitude Pulmonary Edema (HAPE). As someone with no previous respiratory history and a pretty clean bill of health, this was not where I expected to be after what was supposed to be a quick weekend trip to the mountains. What follows is a recap of what led to this point and some information about altitude sickness to increase awareness of this common, but potentially lethal condition.
I flew into Denver (elevation 5,280 ft) from Austin(elevation 498 ft) on Saturday morning 7/24. I hopped in a rental car and drove straight to visit my girlfriend in Silverthorne (elevation 9,035 ft).Naturally, having an IV bar at my disposal, I took the opportunity to get a little IV hydration the day before my flight since I knew I’d be traveling.Unfortunately, I was not aware that being at elevation requires someone to be even more hydrated than one would need to be at sea level. Significantly more hydrated, in fact. In addition to that, the rapid change from 498 ft to nearly 10,000 ft is a huge shock to the system, and it’s much more than just getting winded more easily when you’re taking a walk. I didn’t do anything physically strenuous on Saturday and spent a relaxing evening with adult beverages and TV bingeing.
On Sunday (7/25), we took a short hike in the morning which lasted no more than an hour. There was a slight uphill grade to it, but nothing demanding, and I didn’t even break a sweat. I did notice that I was slightly short of breath during the hike, but I expected that given our altitude. Going back downhill, I didn’t feel short of breath at all. We hung around the house afterward and went to visit friends for dinner that afternoon. It wasn’t until we got back from dinner that I suddenly noticed I had chills and felt really tired. It struck me that I hadn’t felt that way since having COVID in February. So, I just laid in bed and watched TV. But as the evening wore on, I started noticing a little nausea. Was it maybe something I ate? Then there was this intermittent coughing. And then I noticed my heart was beating harder and faster than normal. And then it occurred to me that I was a little short of breath and breathing faster… but why was that happening when I was just relaxing in bed? It wasn’t until I tried to take deep inhales and exhales that I heard and felt the popping and crackling in my chest.
Sometime after medical school, I had read the book Into Thin Air: A Personal Account of the Mt. Everest Disaster, by Jon Krakauer. In it, he described various forms of altitude sickness, one of which was High AltitudePulmonary Edema (HAPE). For some reason, the description of this condition has stuck with me ever since. HAPE typically occurs when “lowlanders” rapidly ascend to 8,000-10,000 ft with early symptoms showing coughing, shortness of breath with activity and a decreased exercise capacity. As it progresses, shortness of breath occurs at rest and people may noticed a faster pulse, faster breathing, elevated body temperature and crackles in the chest. As I was lying in bed feeling all of this, it occurred to me that I either had COVID again (which I thought was unlikely given I was fully vaccinated and these symptoms felt worse than when I originally had COVID), or I had HAPE.
When I woke up Monday morning (7/26), I wasn’t feeling any better. Even sitting up in bed felt like a huge physical undertaking. Walking to the bathroom left me panting. I knew I was supposed to fly back to Austin that evening and was hoping that the 90 minute drive back to Denver and its lower altitude would help me feel better. Now when I coughed, I could feel what felt like a thin, runny, salty fluid in the back of my throat. It felt very distinct from the thick sputum you get with an upper respiratory infection. My shortness of breath and rapid breathing was easily noticeable to anyone who looked at me by this point. Even though my flight wasn’t until the evening, my girlfriend and I decided I would drive back to Denver early to see if it made me feel any better…and if it didn’t she convinced me to go to an urgent care and get checked out before going to the airport. The drive from the mountains to Denver did not make me feel any better. I parked at an urgent care near the airport and the short walk from the car to the building with my mask on almost made me pass out. I couldn’t breathe. The provider in the urgent care took one listen to my lungs and told me to go straight to the ER. In typical doctor fashion, I was being stubborn and wanted to just get on my plane and get back to Austin’s altitude which I knew would take care of the problem. She told me, “Flying right now could very well kill you.”
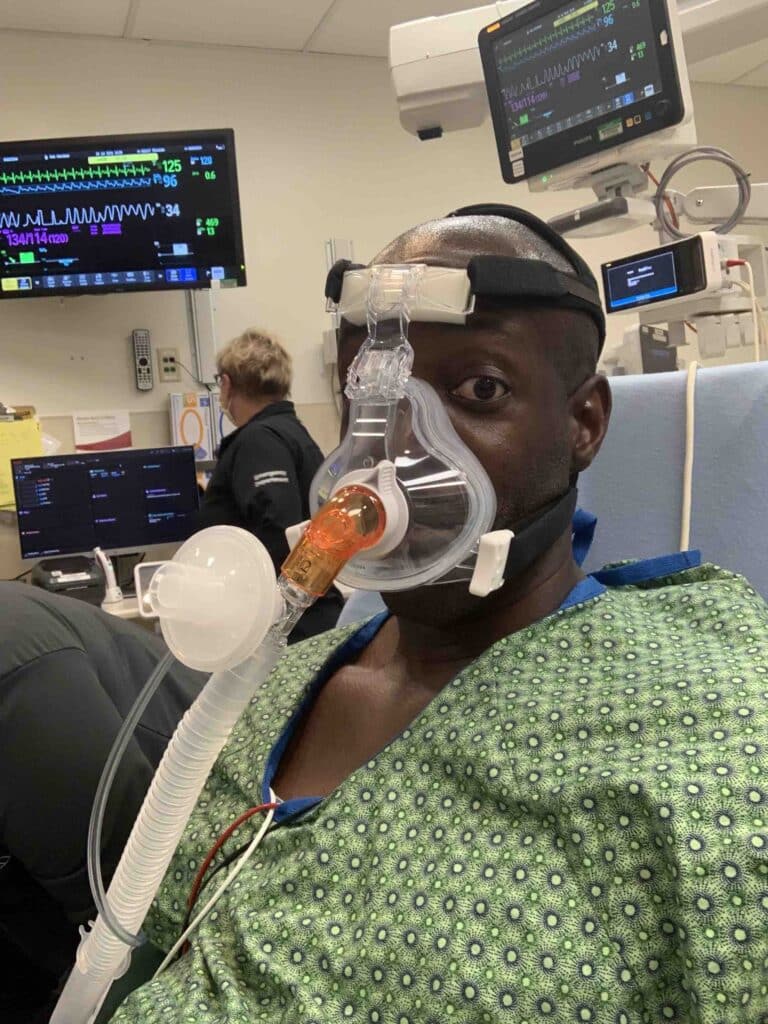
So… I went to the ER and slowly walked up to the triage desk. I told them through gasping breaths what was going on. They directed me to a chair so they could take my vitals. This is when I realized how bad I really was. My pulse was in the 130s, my blood pressure was high… and my blood oxygen saturation was only 55%. I looked at the pulse ox and said, “Is that real?!” The tech looked as shocked as I did and said, “I think so.” He switched the probe to another finger and the number didn’t change. One of the ER docs walked over and took one look at the numbers and said, “We’re taking you straight back.” I was in a wheelchair immediately, and they were rushing me to an ER resuscitation bay where, within 30 seconds, a dozen doctors, nurses and techs were working on me. I had IV lines started, blood drawn for labs, a high-flow oxygen face mask put on me, chest x-rays taken, and people asking me all kinds of questions. After hearing my story of when I got to Colorado, where I’d gone, when my symptoms started and what my symptoms were, they agreed that it was likely HAPE, but they had to rule out other things also. My COVID test was negative (thankfully), and after several minutes of 100% oxygen, my blood oxygen saturation was increasing. They said the needed to admit me to the ICU for constant monitoring to make sure things didn’t take a turn for the worse which would require me being on a ventilator.
And we’re now back to where we began, with me in the ICU wearing a positive pressure mask. All of the other tests they ran on me were negative. I had HAPE. My white blood cell count (which is an indicator of infection or severe inflammation in the body) was 21,000 (normal is less than 11,000). To those of us in the medical field, I would have been described as “sick.” When medical workers say a patient is “sick,” they don’t mean they have a cold or need a hot bath and chicken soup. No, when we say “sick,” we mean “if this person doesn’t get the right intervention quickly, they may die.” When I arrived at the ER, I was “sick.” Choosing not to go to the airport may have been the decision that saved my life, because at the rate I was breathing and with the low oxygen saturation in my blood, I was likely on the verge of respiratory fatigue (when the muscles that control breathing get too tired to function) which would have been followed by respiratory collapse. If that had happened in the middle of a flight…. well, I don’t need to describe the result of that.
Luckily, my hospital course after ICU admission went really well. They were able to wean down my oxygen from 80% down to 30% over the course of the first night while maintaining my blood oxygen saturation above 90%. On day #2, my chest x-ray showed improvement in the patchiness that was seen in both lungs during my initial ER x-ray. They kept decreasing my oxygen requirement, and by the end of the second day, I was able to go about 4 hours on room air (no additional oxygen) with my sats in the upper 80s to low 90s. I was downgraded from the ICU to a regular floor in the hospital where I didn’t need 24/7 monitoring. They put the oxygen back on overnight just because we all breathe less deeply as we sleep, so sats would tend to drop. By the morning of day #3, they were preparing me for discharge with the plan to fly home on oxygen because planes are typically pressurized to the equivalent of 4000 to 8000 ft. I was discharged later that day and spent one more night in Denver just to be safe before flying home the morning of 7/29 with my oxygen generator. From the time I landed in Austin, there was no more oxygen, and I was walking around with sats in the high 90s… I even mowed my lawn that day.
So, how can my experience be beneficial for you?
1. If you’re going to go up to altitudes greater than 8000ft, it’s better to do so gradually, if possible, to let your body adjust.
2. If you do go to altitude suddenly, make sure to be very well hydrated. Drinking 1 to 1.5 gallons of water per day is recommended.
3. If your body isn’t adjusted to altitude, it is best to stay away from alcohol.
4. If you note any of the early symptoms of altitude sickness, seek treatment immediately at the current altitude, or get down to a lower altitude as quickly as possible.
5. Like almost all things in medicine, the best predictor of an event is a prior history of the same event. With this in mind, I now know that I will never venture above 8000 ft on purpose again. I’ve been on that ride, I don’t want to go again.
For those who would like a more clinical description of HAPE, you can find it here:
We are excited to kick off this month by introducing a groundbreaking advancement in testosterone treatment: Kyzatrex, a revolutionary new oral testosterone therapy
Vessel Longevity + IV Bar ATX is committed to delivering the most precise and comprehensive information about IV drips and their function. In this extensive guide, they will probe the complex workings of IV drips, elucidating their operation and their benefits for various health conditions. Whether the reader is a medical professional or someone seeking…